Automatic language translation
Our website uses an automatic service to translate our content into different languages. These translations should be used as a guide only. See our Accessibility page for further information.
The OOHC Health Pathway is a joint initiative of the Department of Communities and Justice (DCJ) and NSW Health aimed at ensuring that every child or young person entering statutory out-of-home care (OOHC) receives timely and appropriate health, assessment, planning, services and ongoing review of their health needs.
DCJ and PSP service provider caseworkers play an essential role in improving the health and wellbeing of children and young people through implementing the OOHC Health Pathway. This guide is designed to help Service Providers to implement the OOHC Health Pathway. DCJ caseworkers are able to access information about implementing the Health Pathway through the DCJ Health Needs of Children in OOHC Practice Mandate for caseworkers.
Research indicates that children and young people in OOHC have increased levels of unmet health need, compared with their peers. A child or young person’s experience of abuse and trauma prior to entering care can significantly impact on their physical, developmental, and psychological health and wellbeing.
All caseworkers have a responsibility to respond to children’s health needs and create opportunities to promote good physical and mental health so they can reach their potential. This will increase children’s prospects and wellbeing into adulthood.
The OOHC Health Pathway was established in 2010 to improve health outcomes for children and young people in statutory OOHC in NSW. The Pathway is a joint initiative of the Ministry of Health and DCJ and is underpinned by a Memorandum of Understanding (MoU) between both departments establishing the roles and responsibilities across the two sectors. The MoU is currently being reviewed by DCJ and the Ministry of Health.
The OOHC Health Pathway aims to improve health outcomes for children and young people in OOHC through the provision of:
The Pathway is supported by an OOHC Health Coordinator employed in each local health district who is responsible for coordination of the health assessment, planning and review process. The key stakeholders that are responsible for implementing the Pathway include the child or young person’s caseworker, the OOHC Health Pathway Coordinator, other health practitioners, carers, birth parents and the child/ young person.
This diagram shows an overview of the OOHC Health Pathway steps and their time frame for implementation. The diagram has been colour coded to show which stakeholders have primary implementation responsibility.
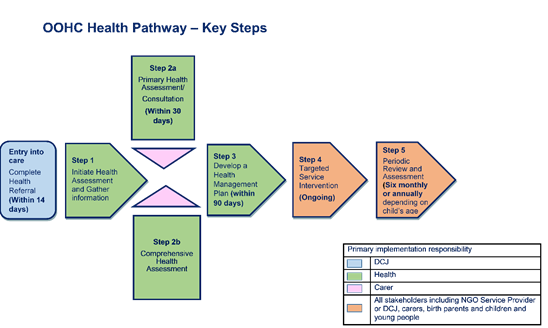
To be eligible to participate in the OOHC Health Pathway children and young people must be in statutory OOHC and the Minister must have parental responsibility for the aspect of the child’s health. Parental responsibility can be either interim or final.
Until recently, the OOHC Health Pathway has only been open to children and young people who entered statutory OOHC after 2010. Recently eligibility for the OOHC Health Pathway has been extended to allow for all children/young people to be referred regardless of when they entered OOHC. If a caseworker is unsure whether a child or young person that they are working with is eligible to be placed on the Pathway, they should contact their OOHC Health Coordinator to find out and discuss the process.
It is important to remember that young people will need to provide their consent to participate on the OOHC Health Pathway.
Children and young people in Intensive Therapeutic Care (ITC) should also participate in the OOHC Health Pathway. The OOHC Health Coordinator and ITC Therapeutic Specialist should work together to avoid duplication of health assessment, planning and service provision.
Each local health district employs an OOHC Health Coordinator. The OOHC Health Coordinator is responsible for coordinating the Pathway process including the assessments that will occur and development of a Health Management Plan for a child or young person.
The way that OOHC Health Coordinators implement the OOHC Health Pathway in their local health district may differ depending on the resources available to them.
The contact details for your local OOHC Health Coordinator are available on the DCJ website. In most instances Health and DCJ Districts align but sometimes they do not. You can use this link to check the Health District that a child lives in.
OOHC Health Coordinators may not necessarily provide caseworkers with a copy of the 2A primary health assessment or advise that it has occurred. Provision of this depends on how their district implements the Pathway.
For children in DCJ managed placements, caseworkers should request contingency funds to cover costs. For children/young people in service provider managed placements services would be funded through the Child Needs Package, or if the issues the child/young person is experiencing are very complex, through application to the Complex Needs Payment.
The OOHC Health Coordinator will be able to provide the caseworker with more information about services in their local health district that are available to meet the needs of Aboriginal children and young people in care. Information about Aboriginal Health Services operating in NSW can also be found on Australian Indigenous HealthInfoNet.
If the OOHC Health Coordinator advises that they do not have capacity to review the Plan because of resource constraints they will advise the caseworker and provide advice about how to get the plan reviewed.
This advice may include that the caseworker use the relevant 2A Primary Health Assessment Form as a guide for review of the Health Management Plan. These forms are available on the DCJ website and are age specific. It is important that caseworker’s do not design their own assessment forms and that the 2A form is always completed by a health practitioner.
Ensure issues identified through the review are investigated and followed up. Request that the GP or health professional who reviewed the Plan organise referral(s) to be made to appropriate follow-up services or ask the OOHC Health Coordinator to make recommendations when they update the Plan.
The OOHC Health Pathway also includes a focus on children and young people aged 15-17 years, accessing the OOHC Health Pathway to commence leaving care planning. The process ensures that children or young people undertake an age appropriate health assessment, and they are linked to adult services. They will also have a Health Management Plan developed that includes strategies to increase their health literacy and any emergency health concerns. The Health Management Plan can be incorporated in the young person's leaving care planning process, to ensure that there are adequate provisions in the young person's Aftercare plan. The assessment may identify the need for further reviews such as NDIS reviews, functional assessments etc, that are best completed prior to turning 18.
An important part of implementing the OOHC Health Pathway is ensuring that the OOHC Health Coordinator is kept informed of any changes to a child or young person’s details. The type of changes that are especially important for an OOHC Health Coordinator to know about include those related to the child or young person’s
OOHC Health Coordinators need this information so that they are aware of which children and young people should be on the Pathway in their district and can work effectively with caseworker’s and carers to meet their health needs.
The caseworker should advise the OOHC Health Coordinator of a change of detail for a child/young person by completing the Change of Details form (DOCX, 81.1 KB) and emailing it to them. Service providers can access this form through the DCJ website. Caseworkers should save a copy of this form in ChildStory or their Record Management System.
Children and young people should be discharged from the OOHC Health Pathway when they leave statutory care. This may occur as they have been restored to their parents, through adoption, guardianship or because of turning 18 years of age.
The caseworker should:
The OOHC Health Coordinator should:
If a child/young person re-enters care DCJ will need to refer them again to the OOHC Health Pathway. This is because they may have experienced violence, abuse or neglect that needs to be considered in a health assessment or have other health concerns.
A child or young person who is deemed a mature minor, must provide their consent to engage on the OOHC Health Pathway. This will generally be from 14, however in some instances may be younger, if you are unsure whether a young person can be identified as a mature minor, contact the OOHC Health Pathway and discuss this with the team. If the child or young person has questions about the OOHC Health Pathway, discuss the key aspects of the program, the importance of having their health needs met, and their right to information. This conversation can be supported by the short video on the OOHC Health Pathway Program located on the NSW Health web page.
If a child or young person in OOHC is a mature minor and they are not consenting to be placed on the OOHC Health Pathway, it is still important that they receive timely assessment, intervention, monitoring and review of their health needs. This can be done by utilising some of the tools used as part of the Pathway without the direct involvement of the District OOHC Health Coordinator.
The caseworker should:
For further information:
See link to online learning module about the OOHC Health Pathway
For questions about implementation of the OOHC Health Pathway or meeting the health needs of children in care email permanency.support@facs.nsw.gov.au
Share information with carers about the OOHC Health Pathway to support them in improving the health outcomes of children in their care: Out-of-Home Care (OOHC) Health Pathway: A Guide for Carers factsheet.
Last updated: